Friday Report: Issue 41
By John Roberts, Dan Ryan and Adele Groyer
COVID-19 Actuaries Response Group – Learn. Share. Educate. Influence.
COVID-19 is still one of the hottest topics for scientific papers and articles. The COVID‑19 Actuaries Response Group provides a regular Friday update with a summary of key papers and articles.
Vaccination
Changes in preventative behaviours after vaccination
One neglected aspect of the media coverage of national vaccine programmes has been the change in behaviour, either in response to your own vaccination or to the increasing proportion vaccinated in your country. Back in January, the Behavioural Insights Team carried out a survey (link) on 3,500 adults on compliance with government guidelines based on how people thought they would act if they were vaccinated (44%) or they were aware that many others around them had been vaccinated (51%) compared with then current attitudes (61%).
A more recent pre-print study (link) in Israel, the undoubted leader in national vaccination programmes, examined changes in preventative behaviours following individual vaccination. Table 1 sets out the changes which show little differences between the sexes, but much higher reductions in social distancing (47%) than mask wearing (21%).
Table 1 – Changes in mask wearing and social distancing behaviour after vaccination

Clotting risks
Potential links between vaccination and elevated risk of cerebral venous sinus thrombosis (CVST) have been in the news and have prompted some governments and regulators to restrict the use of COVID-19 vaccines. CVST is a rare type of blood clot in the brain and If it is coupled with low platelet counts, it can cause bleeding into the brain which can be fatal.
As at 31 March 2021 79 cases of CVST following administration of the Astra-Zeneca vaccine have been reported to the UK’s Medicines and Healthcare products Regulatory Agency (MHRA) (link). Of these, 44 involved low platelet counts and 19 resulted in death. All 79 cases occurred after a first dose of the vaccine, the cases comprising 51 women and 28 men aged from 18 to 79 years. The Winton Centre for Risk and Evidence Communication produced illustrations of the benefits and potential harms of vaccines in terms of risk of ICU admission against risk of CVST against a background of different levels of risk of exposure – low exposure equating to the incidence of COVID-19 during March 2021 and high exposure equating to the peak of the second wave. In a low-exposure scenario they indicated that benefits are likely to outweigh the harms for those ages 30 or older.


Researchers at the University of Oxford used electronic health records from the United States to determine the risk of CVST in the 2 weeks after the following events with the resulting incidence rates shown to the right in Table 2 (link)
Table 2a – Risk of cerebral venous thrombosis (CVT)
| Event | Sample size | Incidence of CVT |
| Diagnosis of COVID-19 | Over 500,000 patients | 39 in a million |
| First dose of mRNA vaccine
– BNT162b2(‘Pfizer-BioNTech’) or mRNA-1273 (‘Moderna’) |
480,000 vaccinated people | 4 in a million |
| First dose of AZ-Oxford vaccine | Reported by European medicines agency | 5 in a million |
Additionally the United States CDC released data from their Vaccine Adverse Evert Reporting System up to 12 April 2021. (link)
Table 2b – CDC data on risk of CVT
| Vaccine | Doses administered | Reporting rate per million doses administered |
| Janssen | 6.86 million | 0.87 per million
6 cases, all with low platelet counts and in women aged 18 to 48 |
| Pfizer-BioNTech | 97.9 million | 0 reports |
| Moderna | 84.7 million | 0.035 per million
3 cases, none with low platelet counts |
The highest rates of CVST have been observed among people who contract COVID-19, so an appropriate balance needs to be struck between benefits of vaccination and the potential harm.
Vaccine Roll-out (link)
The latest weekly data for England continues to show excellent progress with vaccine take-up. For all ages over 55 the first dose take-up is now 94% or higher, and indeed averages 95% for everyone aged 50+. The youngest cohort in Groups 1-9 is proving a little harder to nudge over 90%. This might simply be more difficulty in finding time for an appointment given work commitments, or it could reflect the first signs of the known increased hesitancy in younger age groups. A further possibility is that the publicity around side-effects of the AZ vaccine has had an effect in the last week.
Meanwhile, the focus has switched to second doses, which have recently been up to 80% of the total administered. We can see that good progress is being made with the over 75s despite the reduced overall supply since Easter (which are currently running at around 3m per week, in line with the government’s messaging). Based on the overall position we appear to be around 10 days ahead of the expected 12 weeks delay, suggesting that to date the supply situation for second dose requirements is being managed effectively.

Clinical and medical news
Prevalence of B.1.1.7 variants
The spread of the B.1.1.7 variant, first detected in the UK in September 2020, continues to accelerate in Europe and the USA. The GISAID initiative (link) is gathering data on sequenced viruses from national and international registries around the world, and in particular focusing on COVID variants. Table 3 sets out those countries that have the highest prevalence of B.1.1.7 in their sampled population, whilst reflecting the rate of sequencing is very different across the world.
Table 3 – prevalence of B.1.1.7 variant in sequenced viruses over the last 4 weeks
| Country | All B.1.17 | B.1.1.7 sequenced | Prev (%) of |
| sequenced | in last 4 weeks | B1.1.7 variants | |
| United Kingdom | 202,957 | 33,659 | 98.5 |
| USA | 32,695 | 11,833 | 43.6 |
| Germany | 28,939 | 8,732 | 86.3 |
| Sweden | 10,694 | 2,128 | 94.5 |
| Belgium | 6,369 | 1,385 | 75 |
| Netherlands | 8,456 | 1,272 | 51.5 |
| France | 7,645 | 1,179 | 82.4 |
| Italy | 9,763 | 1,117 | 82.1 |
| Ireland | 6,394 | 938 | 88.7 |
| Switzerland | 5,907 | 928 | 50.4 |
| Spain | 5,203 | 752 | 86.1 |
| Lithuania | 1,573 | 666 | 73.8 |
| Poland | 3,402 | 482 | 77.4 |
Occupational risk for NHS workers
The ONS has previously released a number of publications that look differences in occupational risk from COVID-19 across the population. A new pre-print study (link) has examined differences in occupational risk within the NHS, based on 900,000 employees of NHS trusts between March and July 2020. The study found that COVID-19 sickness absence were lowest at older ages, higher in non-white NHS staff and more than double for registered nurses and healthcare assistance (compared to administrative and clerical staff).
Table 4 sets out the number of COVID-19 cases and odds ratio for different groups over different time periods based on when their NHS trust had cared for 3 COVID-19 cases. The only group to show lower odds ratio when more confirmed cases had been identified were doctors and dentists, although this could be as a result of doctors contracting infections from undiagnosed patients in the early phase of the pandemic.
Table 4 – relative risk of COVID_19 sickness absence for different NHS groups

Data
PHE Life Expectancy Update (link)
PHE has published data which show a fall in life expectancy during 2020 as might be expected. However, it’s important to understand what the data tells us to avoid misinterpretatoin. The life expectancies calculated are for a baby born in 2020 using the age-specific mortality rates seen in 2020 across all ages. These mortality rates are not plausible estimates of the mortality that would be seen through that person’s lifetime, and thus the life expectancies calculated are not in any way ‘true’ (quite apart from not allowing for future mortality improvements since birth).
Nevertheless this measure (known as “period life expectancy”) is useful for a simple comparison of overall levels of mortality between different groups (such as countries, regions, or other factors such as deprivation). Following the links to the tool (link), we can see below how London has been relatively more affected by COVID, falling much more and losing its prior position of highest life expectancy (2019).
By deprivation (not shown in this graph, but available in the tool) we can also see how the gap between the lowest and highest areas of deprivation has widened further, with the latter seeing much greater excess mortality.

Antibody data
We had some inconsistent data on antibody levels this week. First was the ONS fortnightly survey (link), which (surprisingly given continued progress with first doses) showed no overall increase in antibody levels (flat at 55%) , and moreover saw falls in the oldest age groups. There were tentative signs of this in the previous report, but it is much clearer now and extends to younger cohorts too.

With debate over the dosing strategy, and some evidence from other sources that a single dose of the Pfizer vaccine shows reducing levels of antibodies during the extended period between doses, maybe this result should not be surprising after all. However, in contrast, the latest PHE Flu & COVID surveillance report (link) presents a different picture.
In this report, there is no sign of a decrease, with the highest age group having levelled off at around 95%, broadly the level of take-up seen in that cohort.
With second doses for these oldest ages now well under way, hopefully the difference will be relatively short-lived, and we soon see a reversal of the declines in the ONS data. It is worth noting that the ONS does caveat its data to the effect that negative results may be due to antibody levels being present but just at too low a level for the test to detect them. It also points out that other sources of immunity, notably T-cells, may be present, so a negative result does not imply the absence of any protection against COVID.

ONS Infection Survey (link)
This week’s update gives more encouraging news on prevalence levels across the UK. With overall levels much lower, the weekly headline figures for each country have bounced around somewhat, as fewer positive cases result in more statistical variation, particularly outside England, but the chart below shows all four countries firmly trending downwards. These figures are now the lowest since September, at the start of the second wave.
 The ONS has recently restarted providing estimates of new infections, in addition to prevalence. These have been rising, somewhat at odds with the overall picture, but this week is more encouraging, showing a fall from around 15,000 per day in England to 11,100.
The ONS has recently restarted providing estimates of new infections, in addition to prevalence. These have been rising, somewhat at odds with the overall picture, but this week is more encouraging, showing a fall from around 15,000 per day in England to 11,100.
“R” Estimate (link)
SAGE has recently stopped providing an overall estimate of R for the UK, as it suggests that these are less meaningful given different rates of unlocking across the four nations.
 For England, the latest range of 0.7 to 1.0 suggests that the epidemic is still in decline. Regionally, most are caveated that low numbers are increasing the degree of uncertainty, so the estimates should not be relied on alone for policy decisions. As an example the South West is now shown as 0.7 to 1.1, which realistically provides little insight into the true position.
For England, the latest range of 0.7 to 1.0 suggests that the epidemic is still in decline. Regionally, most are caveated that low numbers are increasing the degree of uncertainty, so the estimates should not be relied on alone for policy decisions. As an example the South West is now shown as 0.7 to 1.1, which realistically provides little insight into the true position.
Worldwide excess mortality statistics
Karlinsky and Kobak have released an update to their paper that calculates excess mortality across 89 countries by comparing all-cause deaths from March 2020 against deaths that would have been expected from an extrapolation of deaths observed over 2015 to 2019. The paper can be found at link and ongoing updates can be found at (link).
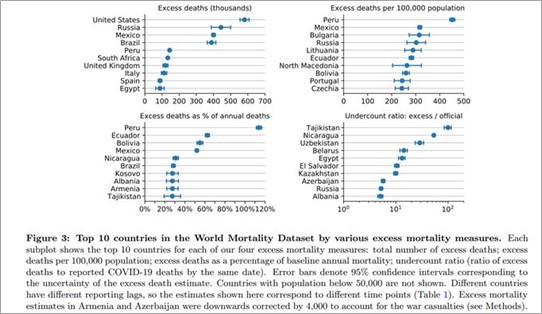
The United States has suffered the highest absolute number of excess deaths at 580,000 including the early months of 2021 (top left table). However, the highest excess deaths as a percentage of expected annual deaths are concentrated largely in South America with Peru at the top of the chart at 114% (bottom left table).
Latin American countries have much younger populations compared to the European and North American countries, which is why the excess mortality per 100,000 inhabitants there was similar to some European countries, but the relative increase in mortality was much higher.
Statistics for a sample of other countries are shown in the Table 5 below and all of these countries include data up to different time points in early 2021.
Table 5 – Excess deaths as a percentage of annual deaths
| Country | Rank by excess deaths as a % of annual deaths | Excess deaths as a % of annual deaths March 2020 to early 2021 |
| Peru | 1 | 114% |
| Ecuador | 2 | 62% |
| Bolivia | 3 | 56% |
| Mexico | 4 | 52% |
| Brazil | 7 | 28% |
| South Africa | 14 | 27% |
| Russia | 15 | 25% |
| Spain | 22 | 21% |
| United States | 25 | 20% |
| United Kingdom | 26 | 19% |
| Italy | 32 | 17% |
| France | 54 | 9% |
| Israel | 55 | 9% |
| Ireland | 61 | 5% |
| Germany | 65 | 4% |
| Denmark, Cyprus, Finalnd, Hong Kong, Macao, Taiwan, South Korea and Thailand | 68 to 84 | No significant change from expected |
| New Zealand | 88 | -6% |
| Mongolia | 89 | -11% |



