Friday Report: Issue 34 COVID-ARG.COM
By Matt Fletcher, Dan Ryan and John Roberts 
COVID-19 Actuaries Response Group – Learn. Share. Educate. Influence.
COVID-19 is still one of the hottest topics for scientific papers and articles. The COVID‑19 Actuaries Response Group will provide you with a regular Friday update with a summary of the key papers and articles that we’ve looked at recently.
Clinical and Medical News
Preliminary findings from Clalit Health Research on vaccine efficacy
Israel has deliberately adopted a simple vaccination strategy of providing vaccines to healthcare workers and all those over age 60. The country is not only leading the world in vaccination uptake, but is demonstrating the power of electronic health records to monitor the efficacy of the vaccine.

Israel is following the two-dose regimen recommended by Pfizer with a separation of 4 weeks. The Clalit Research Institute, linked to one of the four leading patient-funds in Israel, presented preliminary results on Wednesday based on 200,000 matched pairs of vaccinated and unvaccinated individuals over age 60.
While details are limited at this stage, the results appear to concur with the timeline of the Phase III Pfizer trial in that limited to no protection is seen in the first two weeks after vaccination. Thereafter in the following week, the study indicated that the number of positive tests in the vaccinated group fell by between 20% and 40%.
These results are relevant to the UK situation, but only to a limited extent. The vaccination strategy imposed by the UK CMOs stipulates a 12-week separation between the first and second doses of the vaccination. The only active source of data to determine vaccine efficacy over this much longer period will be the electronic medical records of those vaccinated in the UK. As from 11 January, the UK Government has been announcing the number of daily vaccinations (21 Jan: 410,000 received their first dose).
We are already provided with daily updates as to the number of deaths where a positive COVID test occurred in the last 28 days which requires co-ordination of NHS records and death registrations. It would build collective confidence and be no more complicated to provide daily announcements of the number of COVID-19 hospitalisations where the first dose of vaccination took place more than 14 days previously.
COVID Oximetry @home
The COVID Oximetry @home programme was established by NHS England to improve the management of those with positive SARS-CoV-2 tests, and provide a basis for identifying those most in need of hospital treatment. Since the beginning of the pandemic it has become apparent that some individuals with COVID-19 can have very low oxygen saturations without obvious symptoms such as shortness of breath. Failure to identify these individuals early leads to worse outcomes and deaths.
The programme provides patients with a pulse oximeter, and individuals regularly record their results using either a smart phone app, web portal or paper diary. The pilot program started in early December in 4 CCGs, and is being rolled out more widely. Here are links to the most recent data and more information on the programme.
Key questions relate to the further roll-out of the program and what will be determined as optimal trigger levels for admitting patients to hospital.
Modelling
Quarantine and testing strategies in contact tracing for SARS-CoV-2: a modelling study (Quilty et al)
Contacts of confirmed COVID-19 cases are often asked to quarantine for 14 days – this is a significant issue for the individuals involved, which could lead to low adherence. This study looks to assess the merit of testing contacts of infected individuals, to avert onward transmission and reduce or replace the length of quarantine for contacts who turn out not to be infected.
The study finds that either quarantine with a PCR test on day 7 post-exposure or 5 days of lateral flow tests could reduce transmission from secondary cases to similar levels as a 14-day quarantine without testing. However, the authors note that structural issues (delays, poor adherence) reduces the ability of quarantine and testing to reduce transmission, and that these will need to be addressed.
It is important to note that this is a modelling study and hence relies significantly on a number of assumptions about adherence to the various requirements as well as the behaviour of the infection – the authors sensibly note that their findings must be confirmed by studies in real-world conditions before being adopted as policy.
Data
Three-quarters attack rate of SARS-CoV-2 in the Brazilian Amazon during a largely unmitigated epidemic (Buss, Prete Jr, Abrahim, Mendrone Jr, Salomon et al)
The Amazon was the part of Brazil worst hit by COVID-19, which in turn has been one of the countries with the fastest-growing epidemic. This paper focuses on the largely unmitigated spread of the epidemic in Manaus, the largest city in the Amazon region with a population of around 2 million people. These findings give an indication, based on data, of what can happen if SARS-CoV-2 is allowed to spread in a (mostly) uncontrolled way.
A preprint published in September 2020, based on blood samples from bloodbanks in the city, suggested that 66% of the population had been infected. This paper, by the same authors, updates their findings. It finds that the attack rate of 66% in June had increased to 76% in October, confirming that a poorly-controlled outbreak can infect a large proportion of the population.
Whilst few reports of reinfection with SARS-CoV-2 have been confirmed, a population infection rate of over 70% is above the theoretical threshold for herd immunity, suggesting that prior infection may not confer long-lasting immunity. The authors suggest that further studies in the region are needed to investigate the longevity of population immunity and persistence of antibodies, and to determine the need for booster vaccinations.
Household transmission of SARS-CoV-2 and risk factors for susceptibility and infectivity in Wuhan: a retrospective observational study (Fang Li, Yuan-Yuan Li, Ming-Jin Liu, Li-Qun Fang, Dean et al)
This study uses data from the households of confirmed COVID-19 cases and laboratory-confirmed asymptomatic SARS-CoV-2 infections in Wuhan between December 2019 and April 2020, to investigate household transmissibility and risk factors associated with both infectivity and susceptibility to infection. The dataset represents around 40,000 cases, which is 77% of all reported cases in Wuhan as of April 2020.
The study finds that:
- Individuals aged 60+ were at a higher risk of infection than others
- Children and those under 20 were more likely to infect others than adults aged 60+
- Asymptomatic individuals were much less likely to pass on infection than presymptomatic and symptomatic cases
- Household reproductive numbers declined by over 50% following non-pharmaceutical interventions (mass isolation of cases, quarantine of contacts, and restriction of movement)
Given their findings, in particular relating to younger people being more likely to pass on infection, the authors recommend timely vaccination of eligible children once resources are available.
REACT Study
The Imperial College REACT (REal-time Assessment of Community Transmission) study produced its latest report this week on infectivity levels. With a break in surveying from mid-December to 6 January, it acknowledges that it may have missed a peak in late December.
The headline figure is an infection prevalence of 1.6% in the period 6-15 January, slightly less than ONS’ estimates for the turn of the year. Helpfully, 6 January was the start of the latest lockdown.
Possibly surprisingly, it noted that between these dates there is no evidence of a fall, with possibly even the implication of a small increase. This contrasts with other data (ONS, Zoe, PHE) which has showed a fall in infectivity – the difference in their findings has resulted in some adverse comment from observers.
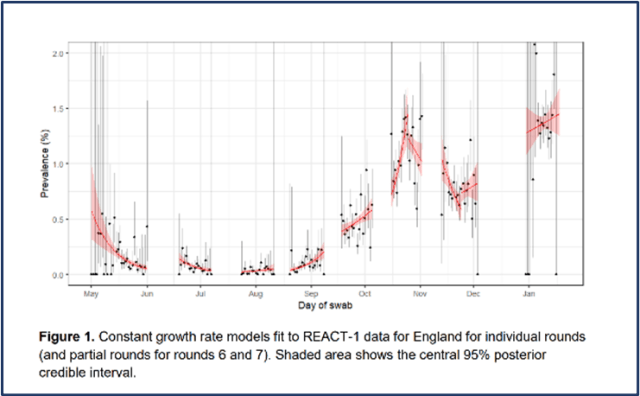 As usual the report has a wealth of information on regional, age and other demographic attributes that make for a very interesting read
As usual the report has a wealth of information on regional, age and other demographic attributes that make for a very interesting read
ONS Infectivity Surveillance
Back after last week’s non-appearance due to data quality issues, as noted above the ONS is suggesting a modest decline in infectivity, albeit with a higher overall figure than REACT of 1.9%. Notable this week is a sharp increase in Northern Ireland – later in the report the reason becomes clear, with the new variant having taken hold in recent weeks, to overtake the original strain.
The regional analysis is now suggesting that London’s peak infectivity was as much as 4% in late December, also driven by the new variant. Although now falling, it remained (at the end date of 16 January) the highest region by some margin.

Public Health England
We noted last week the concerning increase in infections in the over 80 age group, in contrast to falls elsewhere. It’s pleasing to note that the latest report suggests that this group is now falling in line with the overall trend. However, in contrast, outbreaks in care home settings are high.
These two points are of particular interest, as we should very soon start to see the benefits of the vaccination programme, once significant proportions have passed the two week period needed for immunity to take effect.
ONS Antibody Surveillance
Returning to ONS reports, its monthly report on antibody surveillance was published this week, for December. It probably comes as no surprise to see a sudden increase, which will be based on those infected up to and including November. Overall, for England the level of antibodies is put at 12.1%.
 In contrast to previous surveys, the region with highest antibody levels was Yorkshire, although this is likely to be short-lived given the recent surge of infections in London and the wider South East areas.
In contrast to previous surveys, the region with highest antibody levels was Yorkshire, although this is likely to be short-lived given the recent surge of infections in London and the wider South East areas.
Given high levels of infection in December and January, we can expect further sharp increases in the next two months.
“R” Rate
The latest SAGE update of its estimate for R has fallen considerably, at a range of 0.8 to 1.0 for both England and the UK (last week UK: 1.2 to 1.3, England 1.1 to 1.3).
Meanwhile, our own estimate for England has also shown a further fall, although at around 0.95 it is nearer the top end of the SAGE estimate. Our estimate is smoothed however, and so will lag slightly when the underlying rate is moving quickly.

Vaccine Roll-Out
Finally, there’s more encouraging progress in the roll-out of the vaccine, with a further 2m first doses administered in the last seven days. This takes the total to nearly 5.4m by 21 January, representing over a third of the first four priority groups, for whom the target date for completion of first vaccinations is 15 February.
Whilst there have been stories of some areas clearing their first two priority groups and being frustrated at the lack of supply whilst other areas catch up, overall we have a relatively successful start to what will be a mammoth logistical exercise over several months.
Another encouraging sign is the latest survey by ONS on attitudes towards vaccination. In just a month the proportion of those unlikely to accept the vaccination has halved, from 22% to 11%.
And finally …
Vaccine distribution has presented many challenges, but spare a thought for the challenges of the 19th century. The Royal Philanthropic Vaccine Expedition set sail for the Americas from Spain in November 1803. The cargo? Twenty two orphans, deliberately infected with cowpox in order to extract pus from the resultant sores at the end of the voyage to start a smallpox vaccination programme.

22 January 2021





